Welcome to our Learning Lab
Discover all you need to know about probiotics, gut health and more with our interactive learning tools.

What are probiotics?
Not too long ago, the general thought was that all bacteria were bad.
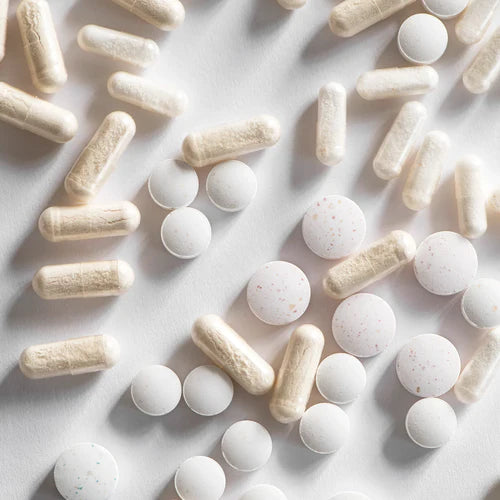
Beyond gut health? The surprise impact of probiotics on your gorgeous smile
From gut to grin! Let’s enter the world of oral probiotics, your new allies for oral health. Here’s three proven ways oral probiotics can help keep your mouth healthy.
Learn moreThe oral microbiome
Just like your gut, your mouth teems with a diverse community of microorganisms known as the oral microbiome.
The peace keepers
Probiotics work like peace keepers in your mouth.
Gassy baby or colic? Symptoms to look for and how to help
Gassy baby or colicky infant? Life with a newborn can be a rollercoaster of sweet smiles and cuddles, combined with grunts, grimaces and restless nights....
Beyond gut health? The surprise impact of probiotics on your gorgeous smile
From gut to grin! Let’s enter the world of oral probiotics, your new allies for oral health. Here’s three proven ways oral probiotics can help...
Probiotics and Babies: A Comprehensive Guide
Probiotics and babies, a comprehensive guide for parents. Discover the fascinating world of the baby microbiome and the best ways to build baby gut health.
Probiotics: A powerful ally for women’s health
Discover the power of probiotics for women’s health! Uncover the science behind these tiny allies, fostering digestive, immune, and emotional well-being.
Gut-healthy foods for a happy Valentine’s Day
Valentine’s Day is just around the corner, and what better way to celebrate than with delicious foods that not only delight your taste buds but...
Your no-nonsense guide to a gut-healthy and bloat-free New Year
'Tis the season to be jolly, but sometimes that joy can come with an unwanted side-effect: the post-Christmas bloat. If you have found yourself feeling...
A guide to moving and eating well during the holidays
As the festive season approaches, the temptation to indulge in rich foods and crash on the sofa becomes more tempting than ever. However, maintaining a...
How does physical exercise influence your gut health and gut bacteria?
It’s well-established that physical exercise is good for health. However, one thing that’s not as commonly known is that exercise also influences the gut microbiota...
What everyone should know about gut health and good bacteria
Your body is home to many trillion microorganisms, including 38 trillion bacteria. Altogether, the bacteria in your body weigh around 2 kg.Until recently, it was...
Meet our Experts

Fatima Kachour
MSc Biomedical Science
Product Development Manager

Julia Tomasson
MSc Engineering Biotechnology
Scientist Microbiology

Jakob Axelsson
PhD Immunology
Research Manager

Louise Ling
Editor-in-Chief
Author

Lucy Upton
Paediatric Dietitian













